Blog
-
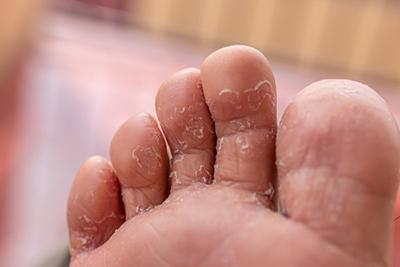
Athlete's Foot: Recognizing and Treating Fungal Infections
posted: May 01, 2024.

-
The Benefits of Seeing a Podiatrist
posted: Nov. 07, 2023.

-
When To See a Podiatrist
posted: Oct. 06, 2023.

-
Why Do People Go to a Podiatrist?
posted: Sep. 14, 2023.

-
Benefits of Having a Podiatrist
posted: Feb. 01, 2023.

-
When To See a Podiatrist for a Sports Injury
posted: Sep. 22, 2022.

-
How A Podiatrist Can Help You With Your Heel Pain
posted: May 19, 2022.

-
The Benefits Of Visiting A Podiatrist
posted: Apr. 14, 2022.

-
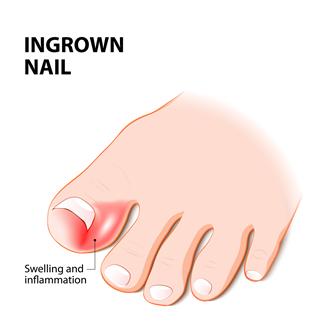
Why You Should See a Podiatrist for an Ingrown Toenail
posted: Jul. 21, 2021.
-
When To See Your Podiatrist For Heel Pain
posted: Jun. 09, 2021.
How your podiatrists in Carmel, Noblesville, Fishers, and Plainfield, IN, can help you get relief from heel painWhen you are experiencing heel pain, it’s easier to think it might go Read more -
What to Expect When You See a Podiatrist
posted: Jun. 26, 2020.
Contact Us
Please enter the following:
Our Location
North West
5471 Georgetown Road Suite C Indianapolis
Plainfield
2230 Stafford Rd. Suite 145 Plainfield
South
8615 US 31 Suite A Greenwood
East
9670 East Washington Suite 215 Indianapolis
Downtown
1801 Senate Blvd. Suite 610 Methodist IU Campus
Carmel
12425 Old Meridian St. Ste A-2 Carmel
North East7950 N Shadeland Ave Suite 100 Indianapolis
7950 N Shadeland Ave Suite 100 Indianapolis
Fishers/Saxony13436 Tegler DriveSuite 100 Noblesville
13436 Tegler DriveSuite 100 Noblesville
