You may have read Dr. Coker’s blog in October regarding post-traumatic arthritis and noticed she mentioned the idea that joints can be fused or sometimes replaced. You may even have had a knee or hip replacement already and were wondering if your ankle may need something too, as it no longer works like it used to.
Yes, we do replace ankles, just like knees and hips are replaced. However, not everyone walking through the door with arthritis in their ankle is a good candidate for an ankle replacement. First of all, an ankle replacement needs to be done by an experienced and certified foot and ankle surgeon, as the procedure is technically demanding. One must be qualified, capable, and willing to deal with any and all potential complications. Secondly, all patients considering an ankle replacement must be thoroughly educated on the risks and benefits of the procedure as well as the post-operative recovery. They must also understand the alternatives as well in order to make a well informed decision. Lastly, it never hurts to obtain a second opinion if you do not feel adequately informed about the procedure.
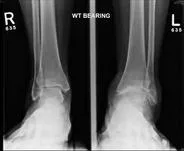
An ideal candidate for a total ankle replacement (TAR) is an individual who is less than 250 pounds, over 50 years old, has no hindfoot deformity, has a lower physical demand, and has severe pain secondary to ankle arthritis. Relative contraindications to a TAR is a high activity level (determined between you and your surgeon), weight greater than 250 pounds, bone loss, osteoporosis, and a history of infection. A patient with diabetes and a history of Charcot Neuroarthropathy, or with an ongoing infection or ulceration should never be considered for an ankle replacement.
A careful look at the literature comparing ankle arthrodesis, or fusion, to a total ankle replacement, shows that the early and intermediate-
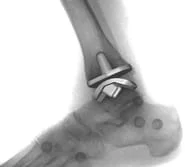
Both an ankle fusion and ankle replacement has its risks and benefits and it is important, that if determined to be a candidate for either procedure, that you understand the potential risks and the long term effects. Ankle replacements have come a long way and can be a very gratifying and beneficial procedure but it certainly is not for everyone. However, if you are suffering from ankle arthritis it is a procedure to discuss with your foot and ankle specialist to determine if it is a procedure for you.
